Head and neck squamous cell carcinoma (LA-HNSCC and Metastatic HNSCC)–Tumour Deck
Price range: $11,800.00 through $20,000.00
The research study conducted by Mellalta Meets provides insights into the Head and neck squamous cell carcinoma covering both LA-HNSCC and Metastatic HNSCC market dynamics, treatment trends, and key opportunities in the G7 regions. It highlights the need for novel targeted therapies, the potential of biomarker strategies, and the significant market opportunity for drug developers targeting the HNSCC population. The study serves as a comprehensive resource for understanding the current landscape and future prospects of HNSCC treatment.
Description
Head and Neck (H&N) cancers primarily targets tumors originating from the oral cavity, including the mucosal lip, pharynx, larynx, and paranasal sinuses. More than 95% of these tumors are squamous cell carcinomas. The most common causes for oral cavity, hypopharynx, larynx, and Human Papillomavirus (HPV)-unrelated oropharynx cancers are tobacco and alcohol use disorders. Patients with H&N cancers, particularly those caused by tobacco and alcohol, risk synchronous primary tumors and developing second primary neoplasms in the H&N, lung, esophagus, bladder, and other sites exposed to these carcinogens.
“Metastatic head and neck cancer is a challenging disease to treat particularly after disease progression on prior therapy, which usually includes radiation and chemotherapy. Over the last 4 years, we’ve seen the big excitement with immunotherapy being approved, with 2 PD-1 inhibitors approved in the recurrent metastatic setting. We’re seeing this moving now to the definitive therapy setting with trials that are accruing.”
Head and neck squamous cell carcinoma is not solely composed of cancer cells but is rather a dynamic ecosystem where tumor cells interact with various components in their microenvironment. This ecosystem includes immune cells, cancer-associated fibroblasts (CAFs), cancer stem cells (CSCs), vasculature, and viral factors such as human papillomavirus (HPV). Understanding the interactions and crosstalk between these components is essential for developing effective treatment strategies.
The relative higher incidence of advanced stage tumours could be related to limited symptomatology in patients with early stage or swift progression from early to advanced stage in HNSCC tumours. Up to 40% of cN0 necks harbor occult metastatic disease. Hence, developing tumour biomarkers to detect metastasis at early stage is essential. Tumour markers play a significant role in secondary prevention. Tumour differentiation can be quantified using biochemical and immunological representation as tumour markers. Currently, the FDA has approved 28 biomarkers after robust in vitro tests for clinical use. However, there is no protein or mutation marker approved for diagnosis or prognosis in HNSCC by the FDA
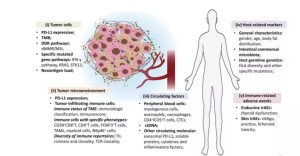
Source: Bai et al, 2020
Mellalta’s Head and neck squamous cell carcinoma (HNSCC) Deck: Current Treatment Landscape
The current standard of care for locally advanced (LA) HNSCC and recurrent/metastatic (R/M) HNSCC involves a combination of treatment modalities, including surgery, radiation therapy (RT), and chemotherapy.
For LA HNSCC, the primary treatment modality is often a combination of surgery and RT. In some cases, multimodal approach is considered in which chemotherapy may also be administered concurrently with RT to enhance its effectiveness.
For R/M HNSCC, the treatment options are more limited. Systemic therapy, which includes chemotherapy and targeted therapy, is the mainstay of treatment. Chemotherapy drugs such as cisplatin, carboplatin, and 5-fluorouracil are commonly used. Targeted therapies, such as cetuximab (an anti-EGFR monoclonal antibody), may also be used in combination with chemotherapy.
Immunotherapy has emerged as a promising treatment option for R/M HNSCC. Immune checkpoint inhibitors, such as pembrolizumab and nivolumab, have shown significant efficacy in improving overall survival in patients with R/M HNSCC.
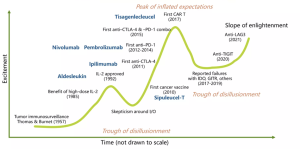
Sell, 2017; Zhang & Zhang, 2020; NCI, 2022; Van den Eynde et al 2020; Buzzatti et al, 2019; Chauvin & Zarour, 2020; Huo et al, 2022;
“Management of early-stage locoregional HNSCC primarily rests on a combination of chemotherapy and radiation therapy. However, the therapeutic trajectory becomes intricate for patients experiencing local or regional recurrence due to radiation field overlaps. Additionally, the management of recurrent or second primary HNSCC has become more complex due to the increased incidence of HPV-associated HNSCC compared to non-HPV HNSCC. This change in disease profile has led to a wider range of treatment options available to practicing oncologists, further complicating the decision-making process.”
Mellalta’s Head and neck squamous cell carcinoma (HNSCC) Deck: Current Unmet Needs
- High rate of disease recurrence and/or metastasis and poor treatment outcomes severely affect long term survival: Over 50% of patients with locally advanced HNSCC who receive multimodal approached develop recurrent or metastatic disease within 3 years of the completing curative-intent treatments.
- Early detection of HNSCC is crucial for better treatment outcomes: Currently, there is a lack of effective screening methods for early detection, leading to a significant number of cases being diagnosed at advanced stages.
- No distinction in treatment strategy for HPV-positive and HPV-negative HNSCC which produces significant morbidity: HPV-positive and HPV-negative HNSCC distinctly differ genetically, they are treated in much the same way, an approach that produces significant morbidity. For patients with advanced-stage HPV-positive HNSCC, the 5-year survival rates are 75% to 80%, whereas fewer than 50% of patients with HPV-negative disease survive for 5 years.
- Diverse cases of Potential ICI resistance mechanisms in R/M HNSCC, which necessitates that many molecular targeted agents be tested in combination with ICIs
“Use of immunotherapy in the treatment of [HNSCC] is still evolving, with a continued unmet need for first-line regimens that provide durable clinical benefit with tolerable safety, further research is needed to determine the utility of dual immunotherapy as a treatment option for [HNSCC] and identify novel biomarkers to predict benefit with immunotherapy.”
Mellalta’s Head and neck squamous cell carcinoma (HNSCC) Deck: Key Takeaways
- Radiotherapy plus concomitant chemotherapy for fit patient’s with unresected LA SCCHN (stage III-IV) has been shown to improve 5-year absolute survival by 6.5% compared with locoregional treatment alone.
- Despite of Cisplatin-Associated Toxicities, Cisplatin remains the radiosensitizer of choice for the majority of patients with locoregionally advanced head and neck cancer.
- Cetuximab is the only targeted therapy that has been proven effective for the treatment of HNSCC in both the LA and R/M settings. The incorporation of cetuximab not only expanded the range of treatment options in the past decade but also encouraged the investigation of many other targeted therapies in this tumor type.
- The current standard of care (SOC) in the second-line treatment of HNSCC typically results in an ORR of approximately 10-18%. There is room for improvement in the effectiveness of existing treatments.
- To be continued…
Mellalta’s Head and neck squamous cell carcinoma (HNSCC) Deck: Questions Answered
- How can anti-PD-1/L1 therapies improve outcomes for patients with locally advanced HNSCC? Which combination strategies involving PD1-based therapies can drive change in recurrent/metastatic HNSCC?
- How can Merck Group’s IAP antagonist xevinapant change the treatment paradigm for locally advanced HNSCC?
- How do oncologists view the role of Adlai Nortye’s anti-PI3K agent buparlisib in the treatment of PD-1-refractory HNSCC?
- What are the key challenges and opportunities in the development of novel therapies for HNSCC, according to KOLs?
- Which companies are best placed to exploit the approach of novel IO-doublet regimens in HNSCC?
Additional information
| Price |
|---|
Table of Contents
- Executive Summary
- Summary of future trends
- Potential opportunities to explore.
- Drivers/barriers for entry
- What’s new in HNSCC.
- Head and neck squamous cell carcinoma (HNSCC) Overview
- Head and neck squamous cell carcinoma (HNSCC) definition, symptoms, etiology, Pathogenesis
- Molecular Alterations in HNSCC
- Head and neck squamous cell carcinoma (HNSCC) Definition & Diagnosis
- Diagnostic Biomarkers
- Diagnostic Algorithm
- Head and neck squamous cell carcinoma (HNSCC) Epidemiology
- Incidence rates by countries
- Stage specific cases of HNSCC by countries
- Head and neck squamous cell carcinoma (HNSCC) Treatment Practices
- Current treatment practices
- Treatment algorithms
- Summarized version of NCCN and ESMO treatment guidelines
- Acceptable endpoints for accelerated approval?
- Head and neck squamous cell carcinoma (HNSCC) Approved Targeted Treatments
- Quick overview of targeted therapies
- Unmet Needs in Head and neck squamous cell carcinoma (HNSCC)
- High rate of disease recurrence and/or metastasis
- No distinction in treatment strategy for HPV-positive and HPV-negative HNSCC
- Challenges with the Current Emerging Targeted Therapy
- To be Continued…
- Pipeline clinical trials
- Head and neck squamous cell carcinoma (HNSCC) pipeline landscape overview and analysis
- Clinical Development of Molecular Targeted Therapy
- Key molecules in clinical trials and results
- Timeline of key drug approvals and launches.
- Phase III Assets
- Clinical trials and results
- Phase II Assets
- Clinical trials and results
- Phase I Assets
- Clinical trials and results
- Head and neck squamous cell carcinoma (HNSCC) Pipeline Early-Stage Molecules
- Phase I and Phase I/II molecules
- Mechanism of action, trial dates, and topline results
- Head and neck squamous cell carcinoma (HNSCC) Pipeline Non-clinical Molecules
- Pre-clinical molecules
- Mechanism of action, catalyst dates, and events
- Physicians/KOLs Input
- Insights from 4 KOLs in the US, EU, and Japan
- Key Catalyst Events in Head and neck squamous cell carcinoma (HNSCC)
- Expansion of approved targeted therapies
- Creation of new actionable targets
- Head and neck squamous cell carcinoma (HNSCC) Market Forecast -2033
- Market Forecast and patient share by key drugs
- Appendix
You may also like…
-

Head and neck squamous cell carcinoma (HNSCC)| Primary Research (KOL’s Insight) | Market Intelligence | Epidemiology & Market Forecast-2033
Price range: $7,500.00 through $22,500.00Select options This product has multiple variants. The options may be chosen on the product pageAccording to Mellalta Meets Analyst’s most recent estimate, the Head and neck squamous cell carcinoma (HNSCC) therapeutics market for HNSCC s was worth US$ Billion in 2023 and is predicted to grow at a 13.9% CAGR to reach US$ 7.5 Billion by 2033.
 English
English